References for CSA 2026 Annual Meeting: Scheduling and AI
References cited in the presentation:
- NASA. What is Artificial Intelligence? [Internet]. [cited 2026 Apr 6]. Available from: https://www.nasa.gov/what-is-artificial-intelligence/
- Oremus W. He spent decades perfecting his voice. Now he says Google stole it. The Washington Post [Internet]. 2026 Feb 15 [cited 2026 Feb 15]. Available from: https://www.washingtonpost.com/technology/2026/02/15/david-greene-google-ai-podcast/
- Fadel L. Former “Morning Edition” host accuses Google of stealing his voice for AI product. NPR [Internet]. 2026 Feb 17 [cited 2026 Apr 2]. Available from: https://www.npr.org/2026/02/17/nx-s1-5716055/former-morning-edition-host-accuses-google-of-stealing-his-voice-for-ai-product
- Chayka K. Is A.I. Art Stealing from Artists? The New Yorker [Internet]. 2023 Feb 10 [cited 2026 Mar 31]. Available from: https://www.newyorker.com/culture/infinite-scroll/is-ai-art-stealing-from-artists
- Generative AI is a marvel. Is it also built on theft? The Economist [Internet]. [cited 2026 Mar 31]. Available from: https://www.economist.com/business/2024/04/14/generative-ai-is-a-marvel-is-it-also-built-on-theft
- Revealed: how academics are being deepfaked on TikTok and Instagram to promote supplements – Full Fact [Internet]. 18:45:23.581133+00:00 [cited 2026 Feb 15]. Available from: https://fullfact.org/health/academics-deepfaked-tiktok-wellness-nest/
- Myers SL, Callahan A, Rosenbluth T. The Doctors Are Real, but the Sales Pitches Are Frauds. The New York Times [Internet]. 2025 Sep 5 [cited 2026 Feb 17]. Available from: https://www.nytimes.com/2025/09/05/technology/ai-doctor-scams.html
- Whyte J. AMA CEO: Deepfake doctors are a threat to public health. STAT [Internet]. 2026 Feb 17 [cited 2026 Feb 17]. Available from: https://www.statnews.com/2026/02/17/deepfake-doctors-scam-ama/
- Harris T, Blakely R. Publisher under fire after ‘fake’ citations found in AI ethics guide [Internet]. 2025 [cited 2026 Feb 15]. Available from: https://www.thetimes.com/uk/science/article/ai-ethics-guide-citations-nsnjmz25b
- Klee M. AI is Inventing Academic Papers That Don’t Exist — And They’re Being Cited in Real Journals. Rolling Stone [Internet]. 2025 Dec 17. Available from: https://www.rollingstone.com/culture/culture-features/ai-chatbot-journal-research-fake-citations-1235485484/
- Walters WH, Wilder EI. Fabrication and errors in the bibliographic citations generated by ChatGPT. Sci Rep. 2023 Sep 7;13(1):14045. doi:10.1038/s41598-023-41032-5
- Anand BN, Wu A. The Gen AI Playbook for Organizations. Harvard Business Review [Internet]. 2025 Nov 1 [cited 2026 Apr 3]. Available from: https://hbr.org/2025/11/the-gen-ai-playbook-for-organizations
Related Reading (in no particular order):
- Marr B. Forbes [Internet]. [cited 2026 Apr 6]. AI: Overhyped Fantasy Or Truly The Next Industrial Revolution? Available from: https://www.forbes.com/sites/bernardmarr/2024/08/15/ai-overhyped-fantasy-or-truly-the-next-industrial-revolution/
- Walsh D. A new look at the economics of AI | MIT Sloan [Internet]. 2025 [cited 2026 Apr 6]. Available from: https://mitsloan.mit.edu/ideas-made-to-matter/a-new-look-economics-ai
- Built In [Internet]. [cited 2026 Apr 1]. What Is Deep Learning and How Does It Work? Available from: https://builtin.com/machine-learning/deep-learning
- Choudhry D. Using AI to create work schedules significantly reduces physician burnout, study shows [Internet]. ASA; 2022 [cited 2026 Mar 27]. Available from: https://www.asahq.org/about-asa/newsroom/news-releases/2022/01/using-ai-to-create-work-schedules-significantly-reduces-physician-burnout
- Gen AI Won’t Make Your Employees Experts. Harvard Business Review [Internet]. 2026 Mar 1 [cited 2026 Mar 8]. Available from: https://hbr.org/2026/03/gen-ai-wont-make-your-employees-experts
- Bedard J, Kropp M, Hsu M, Karaman OT, Hawes J, Kellerman GR. When Using AI Leads to “Brain Fry.” Harvard Business Review [Internet]. 2026 Mar 5 [cited 2026 Mar 8]. Available from: https://hbr.org/2026/03/when-using-ai-leads-to-brain-fry
- Medscape [Internet]. [cited 2026 Apr 6]. Should Doctors Strike to Limit AI Use at Work? Available from: https://www.medscape.com/viewarticle/should-doctors-strike-protect-their-jobs-against-ai-2026a10009vg
- Stackpole T. LLMs Are Manipulating Users with Rhetorical Tricks. Harvard Business Review [Internet]. 2026 Mar 18 [cited 2026 Apr 7]. Available from: https://hbr.org/2026/03/llms-are-manipulating-users-with-rhetorical-tricks
- Chatterjee R. AI in the mental health care workforce is met with fear, pushback — and enthusiasm. NPR [Internet]. 2026 Apr 7 [cited 2026 Apr 8]. Available from: https://www.npr.org/2026/04/07/nx-s1-5771707/mental-health-care-workforce-artificial-intelligence-ai
- Kannarkat JT, Abraham PA, King JS. Workflow Blocking in Clinical Care: The Usability Gap Beyond Information Blocking. JAMA. 2026 Apr 8. doi:10.1001/jama.2026.3249
- Ullah W, MD. Opinion | Replace Yourself With AI, CEO Katz [Internet]. 2026 [cited 2026 Apr 10]. Available from: https://www.medpagetoday.com/opinion/second-opinions/120627
ASA Candidacy
This past October, I ended up tossing my hat in the ring to run for the Vice-Speaker position at the American Society of Anesthesiologists (ASA), for election in October 2026.
The Vice-Speaker and Speaker serve as the parliamentarians for our Board of Directors and House of Delegates meetings. The role includes ensuring that everyone’s voice is heard and that debate is robust but fair to all attendees.
I was the Vice-Speaker and Speaker for the California Society of Anesthesiologists (CSA) between 2011-2018, prior to becoming President-Elect and President.
My campaign-specific website is at drdoyle4asa.com. Check it out!

The frustrations of plugins
Posting, so that someone else won’t have to work quite as hard to solve this problem.
I created a new website, installed the Wordfence plugin (version 8.1.2), got my license key for the site, installed it, and I keep getting the “Wordfence installation is incomplete” with the banner across the top of the screen. Even after entering the license key repeatedly.
Opening the console did not show any errors.
I cleared my cache, turned off all my other plugins, rebooted both Chrome and computer. Nothing changed.
Finally, I deleted the Wordfence plugin with all of the associated data and tables, and then reinstalled it. And it immediately started working.
Tracing my Italian family
The family has long talked about visiting Italy and our grandparents’ hometown. With changes in Italian law, one can claim (reclaim?) Italian citizenship through either the paternal or maternal line. So, down the rabbit hole to collect a variety of records and see what we all might be able to do.
Step 1: See if we can find the ship manifests for when each of my grandparents came to the US. We know the year for each of them. Family lore indicated that Pappa, at least, came in through New Orleans. But we didn’t know where Mamma came in — New Orleans or New York or another port.
We found Pappa on the SS Plata, which went from Palermo to New Orleans in 1891. And then Mamma on the SS Spartan Prince, from Naples to New York in 1898 with her mother and sister and cousin. All of these records are difficult to read.
Step 2: Pull up the copy of the marriage license that I made back in med school. The Omaha public library has a great family history section, and I found that it was a double wedding with one of her sisters. The two licenses also gave me a bunch of other family names.
Step 3: Figure out if either of them were naturalized citizens. This is the hard step, because before 1906, there was no central process or location for records. Naturalization could happen in local, district, state, or federal courts. And most of this is not available on-line. Notations on Census records may or may not be accurate. So there may be a trip to Omaha or the National Archives in Kansas City in our future.
Step 4: Verify all of the US Census records, through 1950 (the most recent year that’s available). This has been the most interesting yet tricky thing, because the family name has been spelled 4 different ways between 1900 and 1950. Pappa’s name is 4 different spellings, and Mamma’s is 3. I finally found them in the 1950 census by searching for their address!
Step 5: Now the hard part – finding records in Italy. This requires professional help. And time.
Harassment, Incivility, and Disrespect references
This presentation has appeared in various formats at various meetings, and the reference list has changed slightly as new information is published. The meetings include: CSA Winter Seminar 2025 (January 2025), ASA ADVANCE (January 2025), Vituity Partnership (September 2025), ASA Annual Meeting (October 2025), Post-Graduate Assembly (PGA, December 2025), ASA ADVANCE (January 2026). Most of these are journal articles, but there are some from the lay media.
ASA. Statement on Harassment, Incivility, and Disrespect [Internet]. 2024 [cited 2025 Jan 12]. Available from: https://www.asahq.org/standards-and-practice-parameters/statement-on-harassment-incivility-and-disrespect
Afonso AM, Cadwell JB, Staffa SJ, Zurakowski D, Vinson AE. Burnout Rate and Risk Factors among Anesthesiologists in the United States. Anesthesiology [Internet]. 2021 May 1 [cited 2021 Aug 20];134(5):683–96. Available from:
https://pubs.asahq.org/anesthesiology/article/134/5/683/115466/Burnout-Rate-and-Risk-Factors-among
Davis K, Pinto JK. The Corruption of Project Governance Through Normalization of Deviance. IEEE Transactions on Engineering Management [Internet]. 2024 [cited 2024 Jan 30];71:2447–61. Available from: https://ieeexplore.ieee.org/document/9826419
DeMaria, Samuel. The Invisible Cut: Incivility’s Silent Toll on Healthcare. 2025.
ISBN: 979-8294912680.
Hastie MJ, Mittel A, Raman V, Szokol J, Whittington R, Bustillo M, et al. Sexual Harassment in Academic Anesthesiology: A Survey of Prevalence, Sources, Impact, and Recommendations. Anesthesia & Analgesia [Internet]. 2022 Mar 18 [cited 2025 Jan 8];10.1213/ANE.0000000000007282. Available from: https://journals.lww.com/anesthesia-analgesia/fulltext/9900/sexual_harassment_in_academic_anesthesiology__a.1091.aspx
Lautenberger D, Dandar V, Zhou Y. AAMC. 2022 [cited 2022 Aug 8]. Understanding and Addressing Sexual Harassment in Academic Medicine. Available from: https://www.aamc.org/data-reports/faculty-institutions/report/understanding-and-addressing-sexual-harassment-academic-medicine
Lautenberger DM, Dandar VM. The State of Women in Academic Medicine 2023-2024: Progressing Toward Equity. Washington, DC: AAMC; November 2024. Available from: https://www.aamc.org/data-reports/faculty-institutions/report/state-women-academic-medicine
Ligibel JA, Goularte N, Berliner JI, et al. Well-Being Parameters and Intention to Leave Current Institution Among Academic Physicians. JAMA Network Open. 2023;6(12):e2347894. doi:10.1001/jamanetworkopen.2023.47894
Lin DM, Lane-Fall MB, Lea JA, Reede LJ, Gomes BD, Xia Y, et al. Workplace Violence Pervasiveness in the Perioperative Environment: A Multiprofessional Survey. The Joint Commission Journal on Quality and Patient Safety [Internet]. 2024 Nov 1 [cited 2025 Jan 12];50(11):764–74. Available from: https://www.sciencedirect.com/science/article/pii/S1553725024002320
Mashour GA. This Is Not Acceptable. ASA Monitor [Internet]. 2023 Apr 1 [cited 2023 Apr 17];87(4):34. Available from: https://doi.org/10.1097/01.ASM.0000925020.07308.aa
Muse IO, Markowitz SD, Doyle CA, Lin DM. ASA Statement on Harassment, Incivility, and Disrespect: Why, How, What…Why Now? ASA Monitor. 2025 Feb;89(2).
Rabin RC. Hundreds Sue Virginia Hospital and Executives Over Unneeded Surgeries. The New York Times [Internet]. 2025 Dec 30 [cited 2026 Jan 19]; Available from: https://www.nytimes.com/2025/12/29/health/chesapeake-hospital-lawsuit-perwaiz.html
Spitzer Y, Kraus M, Doyle CA. We’re #1… and That’s Bad: Anesthesiology Has the Highest Rates of HID. ASA Monitor [Internet]. 2025 Nov [cited 2025 Oct 23];89(11):12. Available from: https://journals.lww.com/monitor/fulltext/2025/11000/we_re__1____and_that_s_bad__anesthesiology_has_the.3.aspx
Graduation!

It’s official, I now have my Masters in Biomedical Informatics.
Commencement was June 6th, but the quarter didn’t end until the 20th, so grades posted a week or so later, at which point I could truly say I was done.
Our trip to Portland for commencement was a lot of fun. We had a chance to catch up with various folks who have moved there from the Bay Area over the years, and explore the area. It’s a place we definitely would like to visit again.

BMI 525 – Graph Exploration and Brief
Christine Doyle
May 5, 2025
TYPE OF GRAPH:
Bar Chart – aka Column Chart
DATA:
This data set was gathered as a part of a qualitative project involving interviews about organizational behavior. The individual concepts have been grouped into larger code groups. This table shows the most frequently identified concepts, and then specifically highlights the multiple concepts that are grouped into “Communication.”
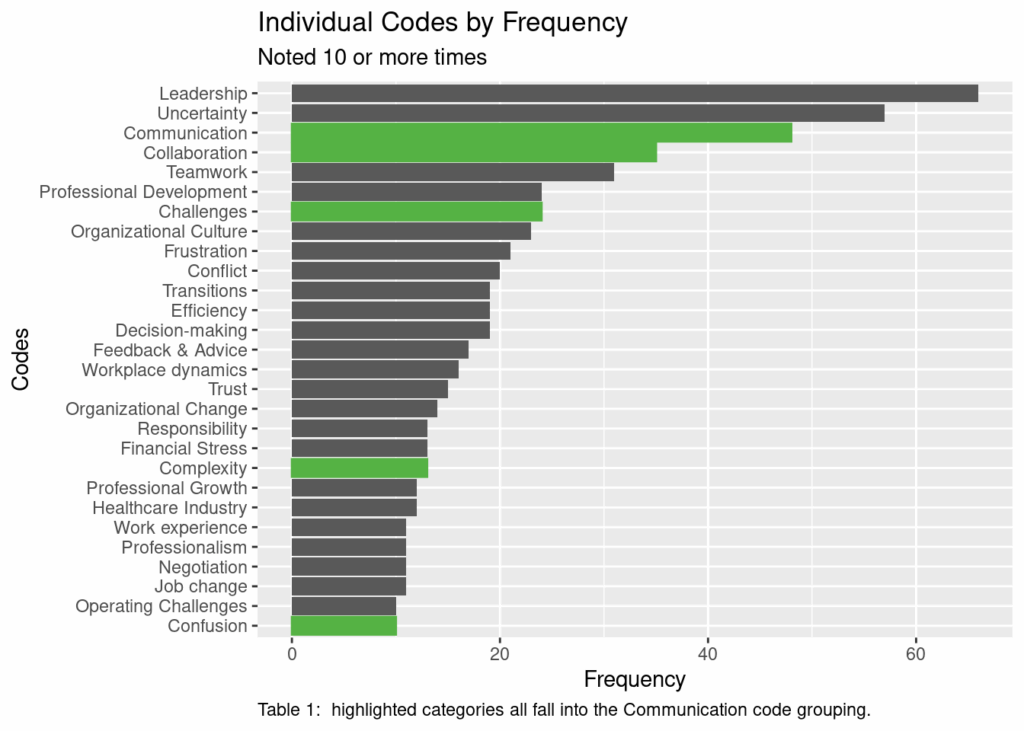
Representation Description:
Bar charts display categorical information on one axis with continuous information on the other axis. The categorical variable may be random or ordered. The ordered variable may be sorted alphabetically or by number or by ascending or descending order based on the other variable. Typical categories might include a graph that has days of the week or locations on one axis (most often the x-axis) against the number of times something falls into that category on the second axis (most often the y-axis). The x-axis and y-axis typically will intersect at the bottom left corner of the chart. If the values are both positive and negative, the axis will be in the center. If the values are all negative, the axis will be at the top.
Bar charts may be oriented with the categorical variable either across the x-axis or y-axis. The orientation of the bar determines if it’s called horizontal or vertical. Horizontal charts have the categorical variable down the y-axis, and are often selected when there are long category labels or a large number of categories.
Bar charts may be grouped or stacked to provide information about two or more categorical variables. Grouped bars may be seen when comparing variable changes between two groups, for example, sales over time. Grouped bars can be easy to use with both positive and negative values. Stacked bars are more often seen when comparing both totals and proportions, particularly looking at change over time or comparison between the different primary categories. Stacked bars are more difficult to use if values are both positive and negative. Stacked bars may also be normalized to the same total height so that the sub-bars become the proportion of that secondary variable.
The bar chart is the most frequently used visualization for non-scientific audiences (i.e., newspaper/press, financial, and government/organizational).
A histogram is not the same as a bar chart, as it is two continuous variables, with one of them divided into groups, although it does look somewhat similar. A line chart is closely related to a bar chart, but implies a continuous progression.
How to Read a Bar Chart:
Simple bar charts should be examined for the order of the categorical variable — is it based on time, based on frequency, or based on something else. This will facilitate understanding of the overall data. Grouped or stacked bar charts should also be examined for the order of the first categorical variable, again looking at time or frequency or something else. If the data is not ordered by time, generally the first categorical variable will be presented in ascending or descending order, and the other variables will remain paired to the first.
Presentation Tips:
Interactivity: Bar charts are not often seen in an interactive presentation. When they are, the goal is to provide additional information about a given category when you select or hover over a particular selection.
Annotation: Annotation showing the exact value of a given variable may be presented overlaying or adjacent the bar. This can facilitate distinguishing between variables with similar amounts, particularly if the scale is condensed and if you are showing stacked bar charts where it is harder to appreciate changes in size of the bar.
Color: Color is often used to distinguish between the different categorical variables. It is most helpful for grouped or stacked bar charts, but can also be helpful in highlighting a specific category or category group.
Composition: The main arrangement decision is how the primary categorical variable is sorted. Dates and times are frequent choices, and may include years, months, days of the week, quarters of the year, etc. Ordering by frequency (either ascending or descending) is also a common arrangement.
Variations and Alternatives
As mentioned above, both grouped and stacked bar charts are variations of the simple bar chart. Depending on the data and time definitions, one might also consider a Sankey diagram.
How to Create it
code_freq <- read_csv(“data/CodeFrequency4Ranalysis1.csv”, col_types = cols()) code_freq <- code_freq %>% janitor::clean_names()
basic_plot = ggplot(code_freq, aes(x=frequency, y=reorder(code, +frequency))) + geom_col() + labs(x = “Frequency”, y = “Codes”) + ggtitle(“Individual Codes by Frequency”, subtitle = “Noted 10 or more times”) + scale_color_hue(c=20) + geom_col(data = subset(code_freq, code_group == “Communication”), color = “#55b244”, fill = “#55b244”) + theme(plot.caption = element_text(hjust = 0)) + # set the left align here labs(caption = “Table 1: highlighted categories all fall into the Communication code grouping.”)
###
Selling Your Hospital, Part 2
This post was originally published on the California Society of Anesthesiologist’s (CSA) webpage on March 7, 2016 With their website rebuild, the archives were not posted.
Home » CSA Online First » Christine Doyle » Selling Your Hospital, Part 2
Selling Your Hospital, Part 2
Mar 07, 2016 by Christine Doyle, M.D.
tags: hospitals

Between the initial announcement of the DCHS sale in October 2014, the conditional approval by the Attorney General on February 20, 2015, and Prime’s withdrawal of its offer on March 10, 2015, we held many meetings. Prime’s operations team visited on several occasions to review our processes and make suggestions. We started implementing some of them immediately, and others later.
 Probably the most important factor that changed was our attitude. We learned how truly important our documentation was for the hospital’s ability to bill for services. We learned about how coders do their work, even if we will never actually do it, so that we could help make their jobs easier. Our medical staff president spent hours one-on-one with our admitting physicians, showing them the difference a single word could make. Most of us had no idea, for example, that “urosepsis” wasn’t a valid diagnosis according to CMS. This information brought secondary benefits as well, as the ICD-10 transition became a non-issue for us.
Probably the most important factor that changed was our attitude. We learned how truly important our documentation was for the hospital’s ability to bill for services. We learned about how coders do their work, even if we will never actually do it, so that we could help make their jobs easier. Our medical staff president spent hours one-on-one with our admitting physicians, showing them the difference a single word could make. Most of us had no idea, for example, that “urosepsis” wasn’t a valid diagnosis according to CMS. This information brought secondary benefits as well, as the ICD-10 transition became a non-issue for us.
Our Geometric Mean Length of Stay (GMLOS), which started out 1.5 days over the target, was reduced to 0.1 days over the target within nine months. Although the actual increase in revenue was not known to us, it was clear that we were appropriately aligning our documentation with what was required by CMS.
We also looked long and hard at our expenses. A mitigation plan, aimed to reduce those expenses, was enacted in April. It was not without controversy, nor was it without revision. Key issues included inaccurate job titles, descriptions, and an overemphasis on confidentiality, leading to crucial positions being eliminated (i.e., our surgery biller) only to be subsequently reinstated. Low-volume service lines were closed or reconfigured.
Communication, once again, became a critically important part of the process. Rumors flew amongst the hospital staff, the local news, patients, other hospitals, and neighbors. Damage control again became important, especially since early advertising had been all about how the hospitals would close if the sale fell through. Fortunately, cash flow improved with receipt of deposit money from Prime and additional state funds.
DCHS filed suit against SEIU and Blue Wolf in Superior Court. Among the complaints were breach of contract for violating the confidentiality clauses, unfair competition by discouraging potential bidders, civil conspiracy for taking action that caused harm to DCHS, and aiding and abetting when Blue Wolf allowed SEIU to influence competing bidders.*
In response, the Attorney General’s office issued this press release, blaming Prime for breaking the deal. Her comments raised concerns that the conditions placed on any other sale would be the same or even more restrictive. These concerns were only slightly appeased when Attorney General Harris stated that “the offer made to Prime was unique and tailored to Prime,” and that conditions for a different transaction would not necessarily be the same.
 Back to square 1 (or maybe 2).
Back to square 1 (or maybe 2).
Within two weeks of the announcement that Prime refused the deal with the Attorney General’s conditions, our agents were again fielding requests from interested parties. The process was the same as before, so much of the work was already done. Our financial situation had slightly improved, and we updated the prospectus. Once again, we engaged in discussions with the Attorney General’s office, and with officials in Paris and Rome, so that when we had a potential buyer we would be able to move in an expedited fashion.
My mother and her neighbors who live within half a mile of the hospital sent letters to Santa Clara Supervisor Ken Yeager and San Jose Councilman Pierluigi Oliverio. They emphasized that the county would suffer a decline in tax revenue and other negative financial implications if businesses (physician offices) moved away from the area when O’Connor became “Valley North.” They asserted that property values would decline in one of the oldest, exclusive neighborhoods in San Jose. No response was received, and both Yeager and Oliverio remained remarkably silent on the entire situation.
The selection committee was reconstituted, with the addition of Sister Margaret Keaveney, who had been named the CEO of O’Connor Hospital after the planned departure of the prior CEO. It turned out that the original committee had no direct representation from the hospitals. Some observers felt that such representation might have improved the bid process and timeline.
After mostly behind-the-scenes machinations, an announcement was made on July 17, 2015, that the selected buyer would be Blue Mountain Capital in conjunction with Integrity Healthcare. The former would provide the capital and the latter the management. Key provisions of the plan included maintaining the hospitals as non-profits for at least three years, keeping them open for at least five years, and conversion of the “church plan” retirement fund to an ERISA-compliant fund.
Both parties had been involved in the original bid. Integrity had been one of the finalists, but had been unable to secure funding in a timely manner. This new combination afforded each the opportunity to play to their strengths. The management team, with whom we would be working, was comprised of executives with extensive experience in California managing both community and academic hospitals.
The paperwork was submitted to the Attorney General’s office on July 31. This meant that the 105th day allotted for public review landed on Friday, November 13. Open hearings were scheduled for the second week in October, and they were much shorter and less contentious. SEIU was remarkably quiet. The final announcement from the Attorney General’s office was made, after a short extension, on December 3. The conditions were as expected, and were accepted by Blue Mountain/Integrity.

On December 14 at 10 am, the formal transfer took place, and we became Verity Healthcare.
______________________________
*Media references to the lawsuit:
http://sternburgerwithfries.blogspot.com/2015/03/seiu-uhws-dave-regan-and-blue-wolf.html
http://www.modernhealthcare.com/article/20150225/NEWS/150229929
http://www.wsj.com/articles/when-unions-trump-hospitals-1426721146
http://www.mercurynews.com/news/ci_29250106/daughters-of-charity-health-system-closes-deal-with-hedge-fund
Selling Your Hospital, Part 1
This post was originally published on the California Society of Anesthesiologist’s (CSA) webpage on 2/29/2016. With their website rebuild, the archives were not posted.
Home » CSA Online First » Christine Doyle » Selling Your Hospital, Part 1
Selling Your Hospital, Part 1
Feb 29, 2016 by Christine Doyle, M.D.
tags: hospitals

My anesthesiology group practices at one of the Daughters of Charity Health Systems (DCHS) hospitals, and our members have been working there for over 30 years. In January 2014, the DCHS board announced a search for a buyer for the five hospitals and associated facilities.

Needless to say, everyone was flabbergasted, although it wasn’t news that our health care system was in trouble. Each facility has a significant proportion of patients who are covered by Medi-Cal, although not all of them reached a sufficient percentage to qualify as a “Disproportionate Share Hospital (DSH)” and receive DSH payment adjustment from CMS. The Daughters’ overarching goal of providing care to the poor and needy has tended to keep them running an operating loss budget, while investment revenue has declined to the point that it no longer offsets the losses.
Thus began a two-year rollercoaster process. While we often compare the process to selling a house, there are some significant differences to keep in mind about the process of selling a health system.
After making the decision to sell, and choosing a broker, you have to create a prospectus for your facility or system. This prospectus is made available to potential buyers. Your broker will then collect information from potential buyers, who may be interested in acquiring the entire system or only certain parts. You will have a series of site visits from bidders, and many meetings with hospital administrators and medical staff.
Once you select a bidder, you must get a series of approvals for the sale. As a Roman Catholic health system, DCHS requires approval of the sale by the head of the Daughters of Charity in Paris, and by Pope Francis in Rome. As a California health system, we also must have the approval of Kamala Harris, California’s Attorney General.
DCHS contracted with Houlihan Lokey, a global investment bank with extensive experience in brokering hospital sales. Representatives of the firm came to talk to the medical staff and explain the process. One of the first points they explained was that the names of all potential bidders would be kept private except to the individuals on the selection team, in part to avoid outside attempts to influence the process. The names of the other bidders would become public when DCHS announced the selected bidder. Houlihan Lokey expected this phase, including on-site visits and due-diligence research by both sides, to last about six months.

Simultaneously, we began working with the Attorney General’s office and with officials in Paris and Rome. We knew that there were likely to be political ramifications of the sale, but we had no idea what they might be.
One of the overarching goals was to sell the system intact, because breaking up the system would have significant financial implications for the three different retirement funds. A break-up of the system would force a conversion of the existing church pension plan, which wasn’t covered by federal laws, to an ERISA-compliant plan, at a projected cost of about $200 million. The Daughters were adamant about protecting these funds both for current and retired staff.
As the summer progressed and the timeline slipped a bit, we started to hear rumors that one of the bidders was Prime Healthcare Services. The Service Employees International Union (SEIU) immediately contacted the ancillary hospital staff, urging them to oppose the deal. SEIU favored Blue Wolf Capital, a venture capital firm that had been co-founded by SEIU in 2005. The local newspaper printed a series of articles, reporting that the Santa Clara County Health & Hospital System (SCVHHS) wanted to buy O’Connor Hospital in San Jose and Saint Louise Regional Hospital in Gilroy, and that Prime was one of the competing bidders.
We kept hearing that the announcement would be made “soon.” It was finally made on October 10, 2015, as we were all traveling to New Orleans for the ASA Annual Meeting. Prime Healthcare’s bid was accepted at $843 million, in a mix of cash and specified capital investments.
Now the real work would begin.
As part of the requirement to submit the selected bid, as well as the other finalists’ bids, and supporting documents to the Attorney General’s office, the documents were made available online for public review. The documents for O’Connor Hospital alone filled 10 four-inch binders, which were available for a mandatory period of 105 days to anyone who wished to review them. There are also mandatory public hearings, and a site visit by a consultant appointed by the Attorney General’s office to make recommendations for conditions of the sale.
Make no bones about it, this was a POLITICAL decision, and like most political decisions, there were opinions and “spin” put forward by all sides.
The SEIU strongly opposed this deal unless Prime was willing to sign a “neutrality” agreement, which in union language means that the union may enter any facility and organize without any opposing action by management. Employees were divided, with most ultimately siding in favor of the sale.
The California Nurses Association (CNA) initially withheld judgment, but ultimately supported the deal as well. They felt that the sale provided the best option for their members, as it would preserve jobs and protect retirement funds.
Three of the five Santa Clara County Supervisors were vocally opposed to the deal. They serve as the Board of Directors for the county hospital system, which is constantly working at capacity, and acknowledged a clear bias in favor of a sale of the San Jose and Gilroy hospitals to the county.
 The local paper, the San Jose Mercury News, initially opposed the sale to Prime. Early on, SEIU published an invited commentary criticizing the deal, as did the Santa Clara county supervisors. Many people submitted letters to the editor, although only a few from the physicians and nurses were printed. Hospital staff encountered roadblocks in trying to contact the editorial board to tell the other side of the story. The hospital system’s advertisements implied the hospitals would all close immediately if the sale wasn’t approved.
The local paper, the San Jose Mercury News, initially opposed the sale to Prime. Early on, SEIU published an invited commentary criticizing the deal, as did the Santa Clara county supervisors. Many people submitted letters to the editor, although only a few from the physicians and nurses were printed. Hospital staff encountered roadblocks in trying to contact the editorial board to tell the other side of the story. The hospital system’s advertisements implied the hospitals would all close immediately if the sale wasn’t approved.
Public hearings were held the first week of January, nearly a year after the process started. Each facility was scheduled for a four-hour hearing, although all of them went on much longer. O’Connor’s lasted 11 hours! The Deputy Attorney General who was in charge had us sit on the “support” (right) side or “oppose” (left) side in the auditorium. SEIU sponsored a cadre of people who didn’t work at DCHS but who traveled and spoke against the sale at each hearing. One DCHS nurse wryly remarked, “I recognize most of the people sitting to my right, and I don’t recognize anyone sitting to my left.”
Given the sheer volume of documents as well as testimony to review, the Attorney General requested, and was later granted, a two-week extension. Her decision was announced at 5 pm on Friday, February 20. The decision was “Approve with Conditions” — 300 conditions in all. Some of the key provisions included a requirement to keep each of the facilities open as acute care hospitals for 10 years, keeping all current contracts, including some very unfavorable ones with two Medi-Cal HMOs. Another condition required increasing the amount of charity care provided each year, despite fewer people needing it, at least in theory, because of the Affordable Care Act.
Prime spent two weeks reviewing the conditions, and then announced on March 10 that they were withdrawing from the agreement because the conditions were onerous and would set a bad precedent.
Now what?
To be continued…
The Physician as Family Member
This post was originally published on the California Society of Anesthesiologist’s (CSA) webpage in 2012. With their website rebuild, the archives were not posted.
Home » CSA Online First » Christine Doyle » The Physician as Family Member
Nov 12, 2012 by Christine Doyle, M.D.
tags: anesthesiologist, Familiy, Patient

I call my mother to say my plane will be on time, and she tells me “someone” will pick me up, as they’re taking my uncle to the hospital with a BP of 220/120 and a HR of 40. Upon my arrival, I am whisked off to the local hospital’s ICU, where the neurosurgeon is assessing my uncle for surgery for his bilateral hygromas. I ask who the anesthesiologist will be and am told, “it doesn’t matter.”
Right, I think. Duly noted. Receiving the message that, as a patient, who your anesthesiologist is does not matter, really gave me something to think about. As someone who was considering my options for areas of specialty training in medicine, that message didn’t sit well with me. In addition, the comment made me feel uneasy about such an unfriendly, unengaging response to a concerned family member.
Flash forward 10 years. I’m on ICU call while doing my training in anesthesiology at Stanford and my pager goes off at 6:00 am. It’s my mother, telling me she’s taking my father to the ED of the same local hospital—the one where I will be starting on staff in 3 months—because “something is wrong.” I drive the 20 miles and meet them in the ED. We find that he has a ruptured spleen (from his thrombocytosis-induced splenomegaly), and will need surgery. The ED physicians ask who we want to see him, and luckily our first choice surgeon is on call. My future partner, Dr. Larry Sullivan, is the anesthesiologist on call, and I start to relax—just a bit.
I certainly knew by this time that who your anesthesiologist is does matter. I believed it so firmly I had selected it as my specialty. I was also more aware of the inner workings of the emergency medical setting and could assist my family better by asking tough questions and simplifying information.
Flash forward another 10 years. My cell phone rings, and I’m told my godmother is in the ED at my hospital with a stroke. I arrive in the ED, go to the back and the physician taking care of her (the “new guy” whom I haven’t met) says to me “Oh, I should have waited for you to intubate her.” I was glad I wasn’t faced with that option—I know that I can’t be objective in this situation. She has had a significant hemorrhagic stroke and may need surgery after we reverse her anticoagulation. The following day she does go to the OR for decompression. I knew everyone on the surgical team and was able to reassure the family members that she has great medical care.
Each of these experiences was stressful, but for different reasons. In the first, I knew the issues associated with increased ICP and the associated risks of anesthesia, but I didn’t know anyone involved in my uncle’s care, and was just “that surgery intern.” In the second, I was extremely stressed, but Dr. Sullivan made me relax by introducing me to the OR, PACU and ICU staff as “our new partner.” In the third, I was the one calming down everyone else, and confusing the staff as to my role in the ICU, since I was “just family.” It’s a tough and insightful experience to be a physician in the midst of a family medical emergency.
Medical school and residency do not always prepare us well with respect to patient/physician interactions. Simulated encounters, as used more often now, help physicians learn how to talk with patients and their families. As in all things, some of us are better than others. But none of us are taught how to deal with being the family member, or even the patient.
As a physician and specifically as an anesthesiologist, I have taken home several lessons from these various encounters. The first is that it’s much easier to talk with patients and family after you have been in those tough roles yourself—and they will recognize that empathy. The second is that “hello,” “please” and “thank you” go an awfully long way to making things better (just like I was taught in kindergarten). The third is that family members really need things to be explained in concrete terms (not the least of which is how you as an anesthesiologist are an important member of their care team). I found that the biggest thing I did was “translate,” not just from medical terms (which most of my extended family know, being in the business themselves), but to short declarative sentences. I frequently had to ask questions in a way that a short sentence was the only way to answer. And the last thing is that your colleagues will automatically look to you to function as the spokesperson, whether or not that’s appropriate. Be prepared to redirect your colleagues if necessary. Ask the difficult questions for the family members who won’t.
I know that I will be the family member again some day. And while I may be stressed and upset, my earlier experiences will make it easier for my colleagues and me to navigate the care of my loved ones in the future.